Jackrite To
Validation of gait parameters for prediction of Parkinson’s disease progression
Jackrite To presents his work on validating gait parameters to monitor the progression of Parkinson's disease better and improve personalized treatment.
Motivation
Parkinson’s disease (PD) is a disorder that affects the nervous system. In the long term, parts of the brain deteriorate, causing involuntary body movements. The individual's gait is gradually perturbed among the noticeable motor symptoms. The progression and severity of PD symptoms are currently assessed via the Unified Parkinson’s Disease Rating Scale (UPDRS) and the Hoenh & Yahr (HY) scale. This UPDRS consists of subjective ratings in questionnaires filled out by the patient, their caregivers, and the clinician. The clinician uses the HY Scale to assess the severity of Parkinson's disease, which consists of a five-point scale ranging from 0 (no signs of PD) to 5 (most severe).
Since subjective ratings might be inconsistent, there is a growing demand to provide quantitative gait assessments. Gait parameters extracted from wearable digital devices worn by the PD patient have the potential to help with the diagnosis and predict PD progression (Fröhlich, Bontridder, Petrovska-Delacréta, et al., 2022).
Validation of gait parameters
The challenge is accurately validating the gait parameters as digital biomarkers to detect PD and monitor its progression. For that purpose, the clinical disease progression needs to be appropriately modeled. A statistical model (the latent time joint mixed effects model (LTJMM)) that takes into account multiple related disease outcomes, such as the UPDRS score, and monitors their progression over time was used (Li, Iddi, Thompson, et al., 2019). This approach can capture the overall progression of the disease for each patient in a single number on a continuous time scale represented by the latent time.
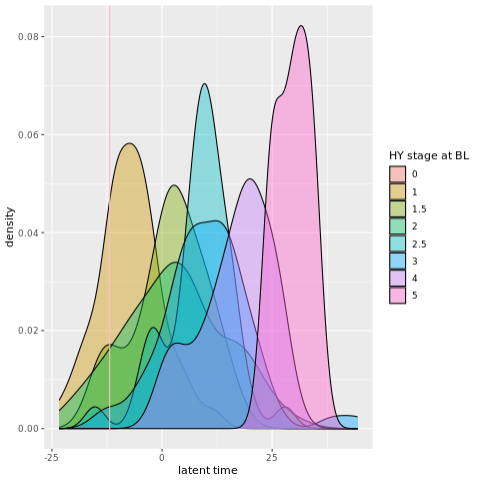
In Figure 1, the HY stage of the patient was not included in the LTJMM. However, each patient’s latent time matches their HY severity stage. So, a patient with a slower latent time indicates a very mild HY severity stage. In contrast, a patient with a later latent time indicates a higher HY severity stage. Thus, the latent time might represent a more granular alternative to the HY scale in monitoring the progression of PD.
Moreover, statistical methods have examined how gait parameters relate to UPDRS ratings. Two main predictors were considered: the Parkinson's patient's latent time and a specific set of gait parameters. The analysis considered whether patients had symptoms mainly affecting the left or right side of their body, as well as the entire patient group.
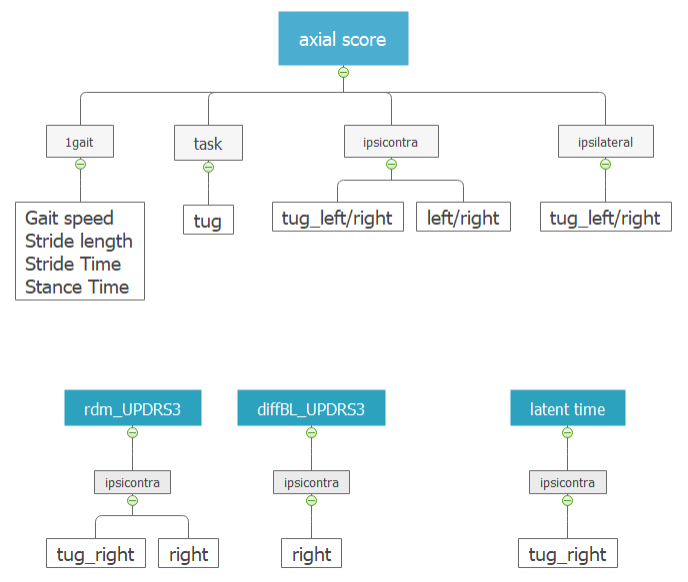
This approach analyzed two sets of patients (Erlangen and NCERPD). In Figure 2, the results showed that various gait parameters (gait speed, stride length, stride time, and stance time) were linked to the axial score (a measure of the overall PD axial symptoms).
By incorporating gait parameters as digital biomarkers, clinicians can potentially obtain more accurate and objective assessments of the motor symptoms experienced by PD patients. These findings may also enable clinicians to monitor the progression of Parkinson's disease more effectively. Tracking gait parameter changes over time allows healthcare professionals to make timely treatment adjustments.
References:
- Fröhlich, H., Bontridder, N., Petrovska-Delacréta, D., Glaab, E., Kluge, F., Yacoubi, M. E., Marin Valero, M., Corvol, J.-C., Eskofier, B., Van Gyseghem, J.-M., et al. (2022). Leveraging the potential of digital technology for better individualized treatment of Parkinson’s Disease. Frontiers in neurology, 13, 788427.
- Li, D., Iddi, S., Thompson, W. K., Donohue, M. C., & Initiative, A. D. N. (2019). Bayesian latent time joint mixed effect models for multicohort longitudinal data. Statistical methods in medical research, 28(3), 835–845.